Medical contribution by Naveed Khan, M.D.,
of Shady Grove Fertility’s Leesburg, VA, office

When you meet with a fertility specialist for your initial consult, he or she will outline for you a diagnostic plan—or infertility work-up—tailored specifically for you, which will help determine the cause of your infertility. The physician will base the testing schedule on the information provided by your medical history and physical examination. This plan will focus on answering many important questions, including the following:
- Are you ovulating?
- Are your fallopian tubes normal?
- Is your uterus receptive to implantation?
- Are the sperm normal in number and function?
The diagnostic tests that comprise the standard infertility work-up answer these questions and help determine the cause of your infertility. While we commonly recommend a set of routine prescreening tests at Shady Grove Fertility, there are some tests that do not always make sense at such an early stage, and we would caution patients from moving in that direction unnecessarily.
Infertility Work-Up: Routine Tests
SGF uses the following standard infertility work-up to evaluate the potential fertility of the female and male partner:
Female
Day 3 Bloodwork
A clinician will perform bloodwork on day 3 of your menstrual cycle to test levels of the following:
- E2 (estrogen): the main female reproductive hormone secreted from the ovary
- FSH (follicle-stimulating hormone): releases from the brain and stimulates the ovary to mature an egg. High FSH levels can indicate to your physician that the hypothalamus and pituitary glands are working harder than normal due to a decrease in ovarian reserve (egg supply). FSH levels can vary from cycle to cycle.
- AMH (anti-Müllerian hormone): AMH is the most accurate predictor of a woman’s egg supply. This test can be more accurate than FSH because there is no fluctuation from month to month and the test is not dependent on a woman’s menstrual cycle, which means women can have the test at any point.
- LH (luteinizing hormone): a hormone that is integral to the final maturation and release of a mature follicle.
Internal Baseline Ultrasound

Embryos implant in the uterus, which makes it necessary to perform tests to determine if a woman’s uterine cavity is normal. A sonographer or physician will perform an ultrasound of the ovaries between days 2 through 4 of your cycle. We use this test to determine the antral follicle count (AFC), which represents the number of eggs available for pregnancy that month.
HSG
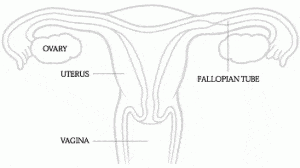
The HSG, or hysterosalpingogram, is an x-ray of the uterus and fallopian tubes to help determine their condition. Physicians rely on this test to see if a patient’s fallopian tubes are open, to assess whether the uterus has normal shape, and to ensure that the cavity is not affected by fibroids, polyps, or scar tissue.
Male
Semen Analysis
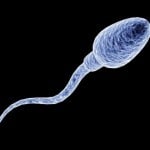
Andrologists perform a semen analysis to evaluate the sperm’s potential to fertilize the egg. The test results will tell your physician the number of sperm in your semen (your sperm count), whether they are normal (morphology), and how well they swim (motility).
Infectious Disease Testing
Through a simple blood test, a clinician will perform infectious disease testing for both the male and female partner.
- Male screening includes: HIV; Hepatitis B surface antigen; Hepatitis C antibody; RPR (serology)
- Female screening includes: Hepatitis B surface antigen; Hepatitis C antibody; HIV; RPR (serology); Rubella titer (one time only); blood group; and RH (one time only). Negative infectious disease results must be documented every 12 months.
Genetic Screening
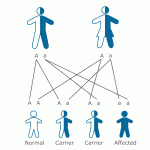
SGF is an advocate for genetic screening when planning for pregnancy, offering testing for over 100 different diseases and syndromes. While we strongly recommend this screening due to benefits for patients and their future children, patients do have the choice to opt out of testing. For patients who are interested, their physician will review their family history at the initial consultation and select the appropriate testing. Patients are provided with a testing kit and will then arrange to return to our center for both partners to be tested during day 3 bloodwork or at specially-scheduled appointment. The testing kit can be run from DNA obtained through either blood or saliva. Once the sample is obtained, the kit is sent out to the genetic testing laboratory, with results arriving to the patient and physician within 2 to 3 weeks.
Infertility Work-Up: Non-routine Tests
The American Society for Reproductive Medicine (ASRM) recommends consulting with your physician to discuss the risks and benefits for any of the tests described below before making a decision. Your personal diagnosis may necessitate one or more of these tests. This article represents a respected clinical viewpoint, but there can be exceptions.
Laparoscopy for Evaluating Unexplained Infertility
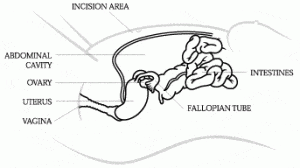
Unless there are suspicions of pelvic conditions based on clinical history, an abnormal pelvic exam, or abnormalities identified through less invasive testing, SGF physicians generally find a routine diagnostic laparoscopy (a surgery that uses a thin, lighted tube inserted into the belly to look at female pelvic organs) unnecessary for patients undergoing an infertility work-up.
Advanced Sperm Function Testing
ASRM found that advanced sperm function testing in the initial work-up—such as sperm penetration or hemizona assays—to generally be unnecessary, as variability exists in these tests with very little correlation between results and outcomes. They are also not cost-effective and can lead to more expensive treatments.
Postcoital Test (PCT)
The postcoital test (PCT) is not easily reproduced and its prediction of pregnancy is “no better than chance,” according to ASRM. Utilizing this test often leads to more tests and treatments, but it does not yield any difference in pregnancy rates.
Blood Clotting Evaluation
Performing thrombophilia tests is of no benefit to patients who do not have any history of bleeding or abnormal clotting, or in the absence of family history. We do not recommend this test as part of the routine infertility work-up.
Immunological Testing
As mentioned above, an infertility evaluation investigates factors affecting ovulation, the fallopian tubes, and sperm, based on clinical history. While immunological factors may influence early embryo implantation, routine immunological testing of couples with infertility is expensive and does not predict pregnancy outcomes.
Prescribe Testosterone or Testosterone Products to Male Partner
Testosterone therapy is widely used for sexual dysfunction, but researchers have found it decreases sperm production, sperm count, and causes infertility. These therapies are not always reversible, even after removing the additional testosterone, so we strongly advise against it if a man is attempting to conceive with his partner.
FSH Level Screening in Women in their 40s
Menstrual cycles for women over 40 are less predictable due to the normal menopausal transition. During this time, FSH levels can vary from woman to woman and from day to day in the same woman. The FSH level will not predict when a woman will transition to menopause or diagnose that it has begun. If there are no other causes of irregular or abnormal bleeding, fertility treatment for women over 40 will not change based on the FSH level.
Endometrial Biopsy
The endometrium is the tissue lining the uterus. This tissue responds to the production of ovarian hormones and allows implantation of the placenta during pregnancy. During menstruation, the upper layers of the endometrium are shed. An endometrial biopsy (removing a sample of this tissue), will not predict the likelihood of pregnancy in general and it is not associated with improved live birth rates in assisted reproductive technology (ART) cycles. Physicians at SGF do not utilize biopsy in the routine evaluation of infertility.
Prolactin Testing in Women with Regular Menstrual Cycles
Prolactin levels are routinely checked during the infertility work-up by many centers. According to ASRM, though, there is no reason to expect that a woman would exhibit significant, elevated prolactin levels when she has normal menstrual cycles and no discharge from her breasts. Therefore, testing prolactin levels in a woman with a normal menstrual cycle provides no benefits and would not impact clinical planning.
Infertility Work-Up: The Bottom Line
When it comes to testing your fertility in the initial work-up, your Shady Grove Fertility physician has your best interests at heart. Day 3 bloodwork, the ultrasound, the HSG, and the semen analysis all provide your physician with important data regarding your reproductive health. Do your hormone levels show a decreased egg supply? Are your fallopian tubes blocked? Does your uterine cavity have a normal shape? Does the male partner have sperm? These are all valid questions that can we can answer from the work-up to help put you on a treatment path that will ultimately lead to parenthood.
If you would like to learn more about the infertility work-up or are ready to schedule an appointment, please speak with one of our New Patient Liaisons at 877-971-7755.





