 British researchers have developed an embryo-incubating system that they say improves odds of conception by 27%. But larger fertility clinics in the U.S. are already ahead of the game.
British researchers have developed an embryo-incubating system that they say improves odds of conception by 27%. But larger fertility clinics in the U.S. are already ahead of the game.
Even with top-notch doctors and top-notch laboratory conditions, pregnancy success through IVF is not a sure thing. So news that a new way of processing embryos during in vitro fertilization (IVF) has enhanced conception rates by more than a quarter would seem to be a welcome development.
At Newcastle University in England, a team of fertility experts has used a system of enclosed, interlinked incubators to more closely control the environment in which fertilization unfolds.
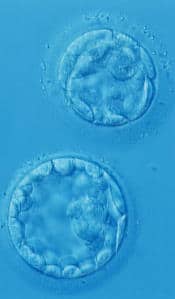
According to research published last week in the journal PLoS ONE, the technique at Newcastle Fertility Centre at Life, part of the Newcastle Hospitals NHS Foundation Trust, yielded a 27% increase in the clinic’s pregnancy rate compared with previous methods in which the embryos were removed from the incubators to assess their progress.
The study compared treatment outcomes over a period of three years, finding that 45% of women achieved a clinical pregnancy — in which a heartbeat is seen via ultrasound at seven weeks of pregnancy – compared with 32% and 35% in each of the preceding two years. “Growing good embryos is the key to IVF success and everyone, even those who have a very small prospect of success, deserve to have the best possible chance,” said Alison Murdoch, a professor of reproductive medicine who leads the clinical service at Newcastle Fertility Centre at Life, in a statement. “Since installing this new technology over 850 babies have now been born.”
The system is indeed innovative in the U.K., where it’s the first of its kind. Researchers reported that it’s been so successful that the same technique has been implemented in IVF clinics in the Netherlands, Canada and Thailand. So why not the U.S.? American women who rely on a boost from assisted reproduction to build their family would surely welcome anything that would improve their chances of conception.
It appears that the larger, more successful U.S. IVF clinics are already using similar methods as well as ones that are even more sophisticated in which controlled video systems provide a window into embryonic development. Incubators that resemble a waffle iron create micro-environments for embryos, which nestle in individual “wells” with little variation in pH or oxygen content.
“Having a well-controlled environment in in vitro fertilization is very important for success,” says Dr. Robert Stillman, medical director of Shady Grove Fertility Center, which has about 15 clinics in the Washington, D.C., metropolitan area.
Participants in the British study were women age 37 or younger who were in the midst of their first IVF cycle and had produced more than 10 ovarian follicles. Ovarian follicles contain an egg; women who produce 10 are considered to have responded well to hormonal stimulation. Their 27% increase in conception is great news for them, but Stillman says that Shady Grove, for example, has a 65% success rate with similar populations.
The average success rate in the U.K. is up to one-third lower than U.S rates, says Stillman, possibly due to differences in health care coverage. In the U.K. where IVF cycles are covered by insurance, women may tend to use their own eggs, which can make pregnancy odds trickier as a patient ages. In the U.S, where IVF is covered infrequently, women may rely more on donor eggs, which can increase pregnancy rates. The U.K. also has more single-embryo transfers, which can lower conception rates.
“They have the right idea,” says Stillman. “If you control the environment, you often get improvements in outcomes with IVF. But would we be able to increase our success rates by 27%? I think we are already toward the max.”
Bonnie Rochman is a reporter at TIME. Find her on Twitter at @brochman. You can also continue the discussion on TIME‘s Facebook page and on Twitter at @TIME.




